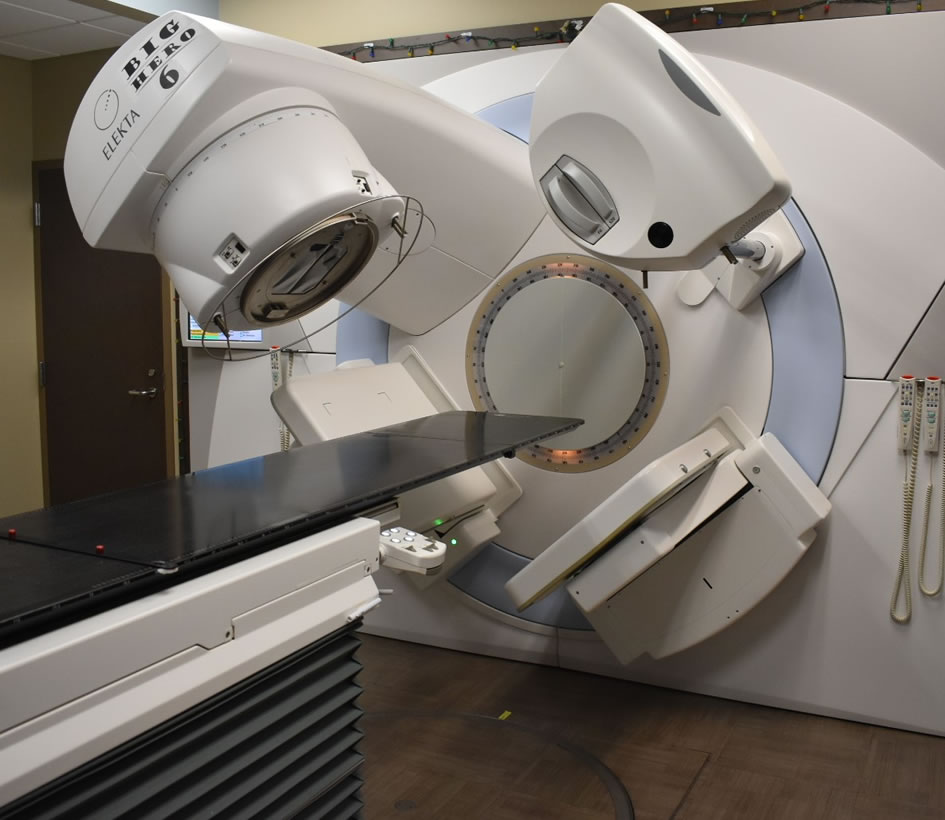
Treatment Process for Radiation Therapy
Consultation
Potential radiation therapy patients will first meet with the physician and the physician assistant. (The physician is a radiation oncologist, a medical doctor who specializes in treating cancer patients with radiation.) The physician and physician assistant will take a medical history and review medical images and test results. A physical exam will be preformed to assess the extent of disease and general well-being. The doctor and physician assistant will explain external beam radiation therapy, its benefits and side effects, and how to care for oneself during and after treatment. This critical first session will be unhurried, probably lasting about two hours. All questions will be answered and all options discussed so the patient can feel as comfortable as possible about the process and make an informed decision as to whether or not to receive radiation therapy.
Many patients who receive radiation therapy experience skin changes and some fatigue. Other side effects are possible, depending on the part of the body being treated. Patients can talk with the radiation team about the likelihood of experiencing various side effects.
Simulation and Treatment Planning
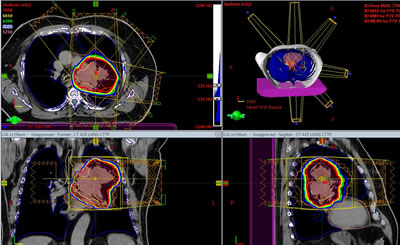 Patients who choose to receive external beam radiation therapy will be scheduled for a planning session called a simulation. During simulation, the patient will lie on a table in the simulation room. The approximate treatment area will be marked by the radiation oncologist or by a therapist under the direction of the radiation oncologist. Immobilization devices, if required, will be made in order to help the patient maintain treatment position during therapy sessions.
Patients who choose to receive external beam radiation therapy will be scheduled for a planning session called a simulation. During simulation, the patient will lie on a table in the simulation room. The approximate treatment area will be marked by the radiation oncologist or by a therapist under the direction of the radiation oncologist. Immobilization devices, if required, will be made in order to help the patient maintain treatment position during therapy sessions.
Computed Tomography (CT) will then be performed in order to visualize exact treatment area placement. The scan will be sent electronically to the treatment planning computer. The radiation oncologist and dosimetrist will then design a detailed treatment plan. Each plan is custom designed for the individual patient so that the beams will conform to the target tissue and maximally protect the normal tissues. After the plan is approved by the radiation oncologist, the information will be entered into a computer system which will transfer it to the treatment machine.
This preparatory work takes some time, so treatments will begin several days after simulation.
Treatment
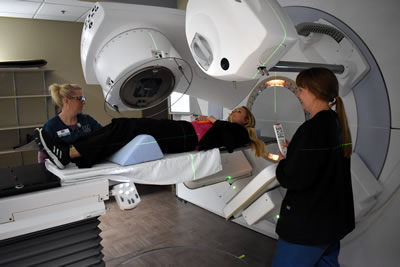 Most patients will receive radiation treatments five days per week, Monday through Friday, for one to eight weeks. However, other schedules may be used. Therapists will help the patient get on the treatment table and position the immobilization devices. Wall lasers will be used to align marks on the patient and immobilization devices to ensure an accurate treatment position. The therapists will leave the room and return to the control console to verify positioning using x-rays in a process called image guided radiation therapy. After all adjustments are made and verified, radiation delivery will be initiated. Closed circuit television screens and an intercom system will be used to monitor the patient during the entire treatment. The treatment itself will only last a few minutes (up to 15 minutes), will be painless, and will not not make the patient radioactive.
Most patients will receive radiation treatments five days per week, Monday through Friday, for one to eight weeks. However, other schedules may be used. Therapists will help the patient get on the treatment table and position the immobilization devices. Wall lasers will be used to align marks on the patient and immobilization devices to ensure an accurate treatment position. The therapists will leave the room and return to the control console to verify positioning using x-rays in a process called image guided radiation therapy. After all adjustments are made and verified, radiation delivery will be initiated. Closed circuit television screens and an intercom system will be used to monitor the patient during the entire treatment. The treatment itself will only last a few minutes (up to 15 minutes), will be painless, and will not not make the patient radioactive.
LINEAR ACCELERATOR - ALSO KNOWN AS "LINAC"
A medical linear accelerator (LINAC) is the device used for external beam radiation treatments. It delivers high-energy x-rays or electrons to the region of the patient's tumor. The therapists will leave the room and return to the control console to verify positioning using x-rays in a process called image guided radiation therapy. Specialized cameras and an intercom system will be used to monitor the patient during the entire treatment. The treatment itself will only last a few minutes (up to 15 minutes), will be painless, and will not make the patient radioactive.
Weekly Doctor Checks
The radiation oncologist and the physician assistant will see the patient weekly to evaluate progress, monitor side effects, and address any concerns. Changes may be made to the course of treatment depending on a patient's response or reaction to the therapy. Patients are encouraged to have another person with them during these visits; having another set of ears to capture the information communicated in these sessions can be very beneficial to patients.
When the course of treatment is finished, the patient will be scheduled to return for a follow-up visit. Additional testing may be required before this visit. The office staff will schedule these tests as needed, and the results will be available for the doctor to review with the patient during the follow-up appointment.